Overview
Epilepsy is one of the most prevalent neurological disorders, and 25-30% of patients with epilepsy have seizures despite multiple attempts at medical management. In those cases, there may be the potential for neurosurgical intervention and even the possibility of complete alleviation of seizures. A remarkable array of new technologies makes surgical intervention more precise, less invasive, and more broadly effective than was possible even just 10-15 years ago.
Epilepsy is characterized by recurrent seizures, which can take many forms depending on the patient and brain circuits involved. Seizures arising from the temporal lobe of the brain, for example, may consist of “staring spells,” lip-smacking and hand fidgeting, whereas those that arise from the frontal lobe may consist of complex, movements of the head, arms and/or legs. As seizures spread from one part of the brain to another, their appearance may change and eventually “generalized” convulsions may occur, which may be associated stiffening and/or repetitive shaking, and with a loss of consciousness. Some types of seizures are generalized from the get-go.
Sometimes the lead-up to a seizure may consist of an “aura,” which is an experience of a certain sensation or emotion (such as a particular smell or sense of anxiety / fear, in temporal lobe epilepsy). After a seizure, patients may experience a “post-ictal” phase in which they feel exhausted and may not have any memory of the event.
Because of the complex nature of epilepsy, determining whether surgery is potentially a good option, and then determining what type of surgery is best, requires an in-depth, highly-specialized evaluation by a dedicated team of epileptologists (neurologists who specialize in epilepsy), neurosurgeons, neuropsychologists, radiologists and others. Brown University Neurosurgery at Rhode Island Hospital is part of a Level 4 epilepsy center (the highest designation available), meaning the full range of diagnostic and therapeutic options are available. We work as a team to design optimal treatment strategies tailored to the condition and needs of each individual patient.
Comprehensive Care Center
Neurosurgical Options
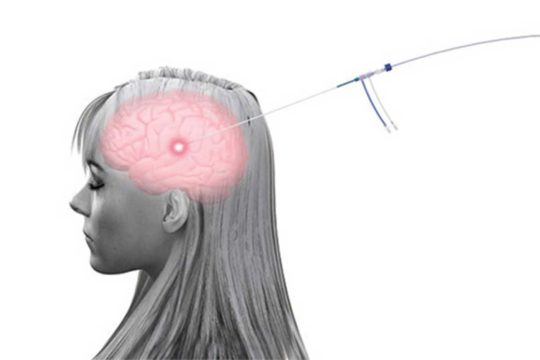
- Minimally-Invasive Laser Ablation
- Responsive Neurostimulation (RNS)
- Deep Brain Stimulation (DBS) of the Thalamus
- Craniotomy for Resection of a Seizure Focus
- Corpus Callosotomy
- Stereotactic electroencephalography (SEEG)
- Subdural electrode monitoring (“grids and strips”)
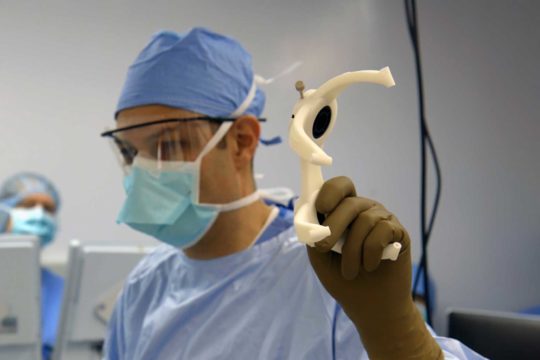
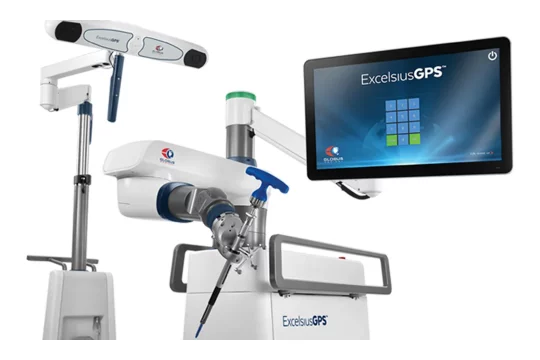
Technology
593 Eddy Street, APC6
Providence, RI 02903
Phone: (401) 793-9166
Fax: (401) 444-2788