Comprehensive Care Centers
Overview
Rhode Island Hospital is a Level 4 (highest level) epilepsy center, offering deep expertise and the full array of the most advanced surgical options for people with epilepsy.
Those with epilepsy not completely controlled by medication may be candidates for surgical treatment. In many cases, surgery can offer the possibility of eliminating seizures where medicines have failed. Individual cases are evaluated by a team of doctors and other clinicians, including neurologists, neurosurgeons, neuropsychologists, radiologists and others, to design patient-specific treatment plans that maximize the possibility of seizure control while minimizing risk. Patient’s individual concerns and preferences play a large role in designing the optimal treatment plan.
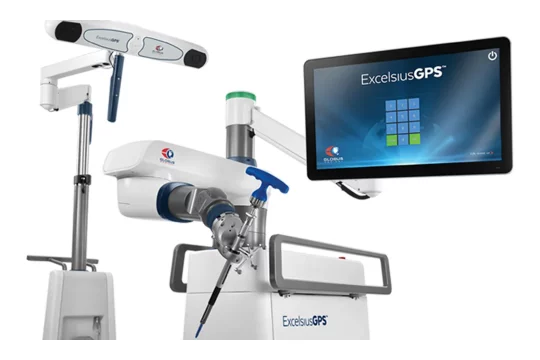
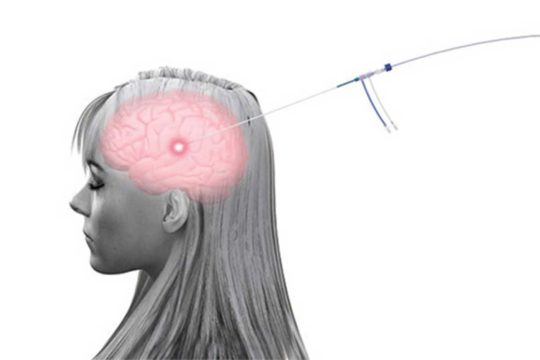
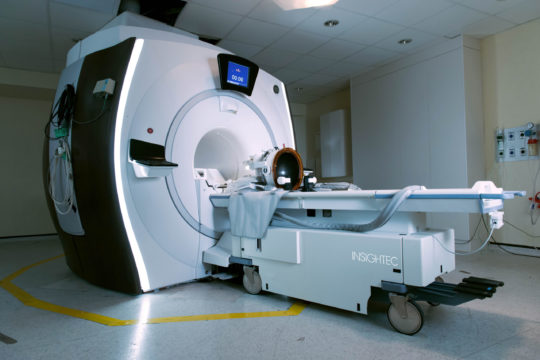
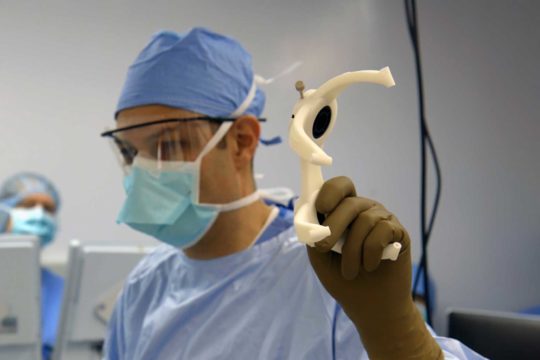
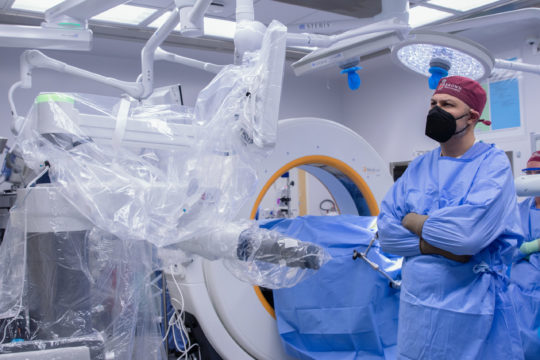
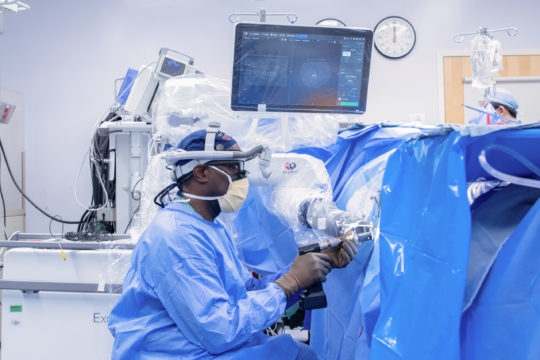
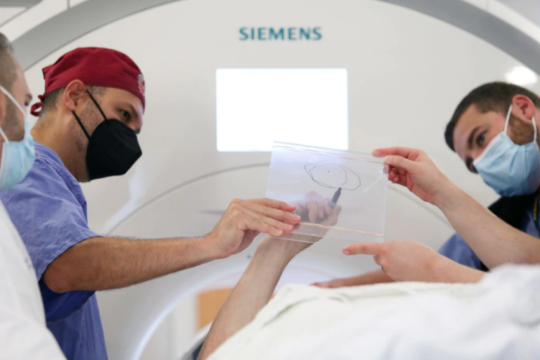
We combine this patient-centered approach with the most advanced technology to deliver the highest-quality, world-class care. These technologies include MRI-guided laser ablation, high resolution pre- and intra-operative neuro-imaging, 3D-printed patient-customized brain targeting systems, high-precision intra-cranial neurophysiology, and responsive (“closed-loop”) neurostimulation systems. These technologies allow us to more accurately identify seizure networks in the brain, and then to deliver optimal treatment.
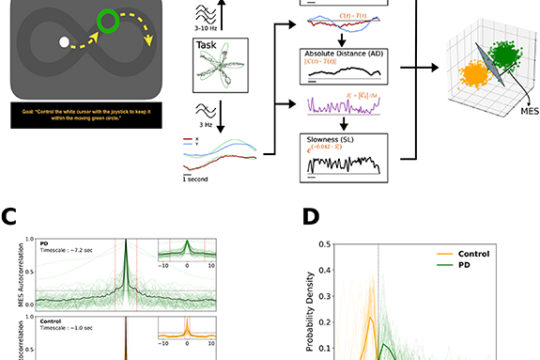
As members of the Brown University faculty, our clinicians not only apply the latest technologies to improve our patients’ lives, but we also conduct research to better understand epilepsy and related problems with cognition and memory, as well as to develop and test new therapies. Ongoing studies focus on the neurophysiology of memory and attention, memory neuromodulation, machine-learning decoding of neural activity, nonhuman models of cognitive processes, and patient-based clinical trials, among many others.
Our talented, highly-experienced team and extraordinary technological resources enable the Brown University / Rhode Island Hospital Comprehensive Epilepsy Program to deliver exceptional medical and surgical care to individuals with epilepsy seeking improved quality of life.
Our Team
Director
Neurosurgery
Neurology
Andrew Blum, MD, PhD, Director, Adult Epilepsy Neurology
Neishay Ayub, MD
John Gaitanis, MD, Director, Pediatric Neurology
Duyu Nie, MD, PhD
Jason Richards, MD
Rachit Patil, MD
Julie Roth, MD
Neuropsychology
Seth Margolis, PhD
Radiologists
Jerrold Boxerman, MD
Glenn Tung, MD
Conditions We Treat
Epilepsy
- Intractable Focal Epilepsy
- Intractable Generalized Epilepsy
Technology
Recent News
Rhode Island Hospital
Ambulatory Patient Center
(APC) 6
593 Eddy Street
Providence, RI 02903
401-793-9128
401-444-2661